 Irvine, CA) and recorded using an Agilent Technologies (Andover, MA) model V24C monitor. Pressures were measured using TruWave pressure transducers (Edwards Lifesciences LLC. The column of water was calibrated and could be automatically adjusted to generate static pressures over a physiologic range of 5 to 25 mmHg. Care was taken to avoid excessive external compression or bending of the catheters at the insertion points. The PICC and control were inserted into the device opposite of each other with the catheter tips at the base of the column of water, allowing simultaneous measurements from the PICC and control catheter. In an in vitro study, we designed an inverted T-device to generate controlled pressures via a column of water. A property unique to the Morpheus catheter is that the shaft transitions from increased stiffness at the proximal end to softer flexibility at the distal end. In addition, PICC length and flexibility, necessary design requirements, intuitively suggest to clinicians that central venous pressure measurement via PICC may not be accurate.įor our study, we selected the AngioDynamics Morpheus PICC. However, there is limited literature on functional accuracy of PICCs for measuring CVP. Interestingly, CVP monitoring is an indication for use for several commercially available PICCs, including those manufactured by AngioDynamics, Arrow, Bard, and Medcomp. 
Peripherally inserted central catheters (PICC) are increasingly used in the hospital setting, and do not have the same risk of complications with insertion as compared to centrally inserted catheters. Ĭentrally inserted central catheters (CICC) and pulmonary artery catheters (PAC) are the current gold standard instruments for measuring CVP, but insertion of these catheters carries the risk of pneumothorax, hemothorax, and severe bleeding. In 2001, Rivers and colleagues demonstrated a sixteen percent reduction in hospital mortality with an early intervention bundle including aggressive volume resuscitation guided by central venous pressure (CVP) monitoring. Despite profound technological advancements in medicine over the last two decades, no intervention has impacted the treatment of severe sepsis and septic shock to the degree of early goal directed therapy. As the country's population grows and ages, the incidence of sepsis is also increasing. Severe sepsis and septic shock are the leading cause of death in non-cardiac intensive care units and the 10 th overall cause of death in the United States. Sepsis is a major cause of death in the world and carries a mortality rate of 20 to 60% depending on the severity of the disease. Clinical studies are required to assess whether the novel PICC has bedside equivalence to conventional catheters when measuring central venous pressures. In vitro, no static or dynamic pressure differences were found between the PICC and a conventional CVP catheter. Dynamic pressure waveforms plotted simultaneously between PICC and control revealed equal peaks and troughs. 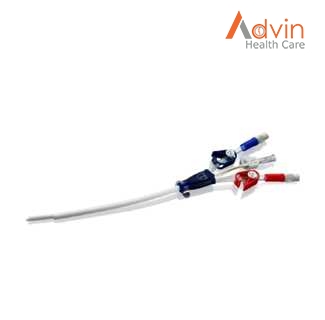
The correlation coefficient for both catheters was 1.0 (p-value < 0.001). The average bias determined by Bland-Altman plot was 0.043 mmHg for 5 Fr PICC and 0.023 mmHg for 6 Fr PICC with a difference range of 1.0 to -1.0. Six-hundred thirty measurements were made using the 5 Fr and 6 Fr PICCs. The resultant PICC and control waveforms were recorded simultaneously. Additionally, random repetitive pressure pulses were applied to the column of water to simulate physiologic intravascular pressure variations. Measurements of static pressures over a physiologic range were recorded using 5Fr and 6Fr dual lumen PICCs. Digital transducers were used to obtain all pressure readings. 
We designed a device to generate controlled pressures via a column of water allowing simultaneous measurements from a PICC and a standard triple lumen catheter. We studied the accuracy of a novel PICC to transmit static and dynamic pressures in vitro. Use of peripherally inserted central catheters (PICC) is increasing, but little data exists comparing a PICC to a conventional CVP catheter. Central venous pressure (CVP) monitoring is essential to guide adequate resuscitation. 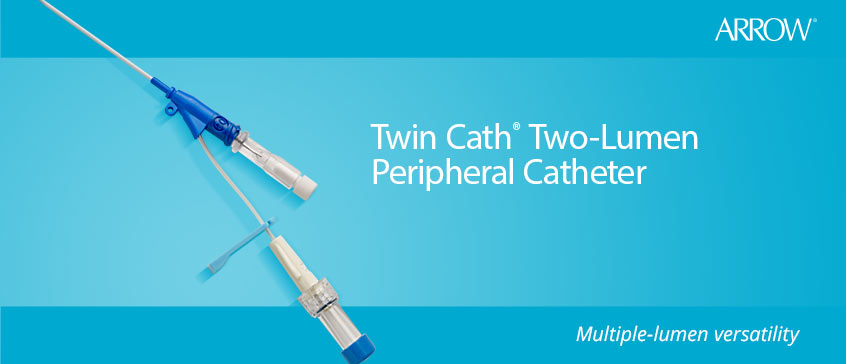
Early goal directed therapy improves survival in patients with septic shock. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
